Newsletters
The header image is the default header image for the site.Dealing with Hurricane Helene – Mission Hospital Asheville NC
POSTED: October 20th, 2025
POSTED IN: 2025 EM Pulse - Q3, EM Pulse - The Official Newsletter of MOCEP,
Written by: Douglas Char, MD FACEP
The Administration for Strategic Preparedness and Response – Technical Resources Assistance Center and Information Exchange (ASPR TRACIE) under the Dept of Health and Human Services, sponsored a webinar on Hospital Disaster Preparedness on August 27, 2025. The presenters were Melissa Cole Harvey, RN, Assistant Vice President, Enterprise Emergency Operations HCA Healthcare and Wyatt Chocklett, CEO, Tristar Horizon Medical Center (Dickson, TN). They shared how they prepared for and responded to Hurricane Helene. Their lessons learned provided thoughtful information for all healthcare providers.
Background Hurricane Helene
On September 26, 2024, Hurricane Helene came ashore in northwest Florida as a Category 4 storm, then stalled out over the southeastern U.S. While the Gulf Coast got walloped, most of the damage was inflicted over the mountains of western North Carolina and eastern Kentucky. Rainfall (up to 31 inches) caused rivers to overflow, produced flash flooding, landslides, and washed-out roads. Helene killed 250 people across six states, but 50% of the deaths were in North Carolina. In Asheville, North Carolina, the effects of fast-moving water and mud cut several of the road and rail links to the town, damaged and destroyed thousands of structures, and severed the pipes that connected Asheville’s water treatment plants, which are in the mountains, to the city itself. Nearly a year later, many impacted communities continue to struggle. One of the bright spots is that the hospitals in the area, while severely damaged, are mostly back up and operational.
Mission Health is an 8-hospital system in western North Carolina, based out of Asheville. HCA Healthcare acquired Mission Health in 2019. Mission Hospital, at 815 beds, is the largest facility in the region and a level 2 trauma center and level 3 neonatal ICU. One doesn’t usually think of mountainous regions as being vulnerable to a hurricane. The hospital lost power and water on the first day of the storm. The sewage system was so backed up that toilets couldn’t be flushed. The area’s water treatment facility was destroyed. At one point, Drummond said, the hospital’s emergency department was double its usual capacity, packed with 200 patients in a facility meant for 100. They ran out of food and supplies within 24 hours. After a few days, the response kicked in. Two hundred thousand gallons of water per day were trucked in to support the facility. During the first week, HCA dug a well to supply the hospital with water. HCA has its own corporate disaster planning group. The Health System brought in over 600 personnel (400 nurses, 50 physicians, 50 incident response team members, 4 behavioral health teams) and equipment from outside the area to support Mission Hospital.
The federal response included sending Disaster Medical Assistance Teams (DMATs) to hospitals in Asheville (Mission Health Hospital), Spruce Pine (Blue Ridge Hospital), Mills Springs, and Hickory North Carolina. I was privileged to be part of this effort as the CMO for Hurricane Helene (during the 2nd week), and then Hurricane Milton rolled into Florida. HHS set up a mobile emergency department in the Mission hospital parking lot to help offload the facility. It turned out to be the largest clinical footprint in NDMS history and included X-ray and laboratory capabilities. DMATs worked in conjunction with HCA providers at Asheville and Spruce Pine. The DMATs were operational for close to a month.
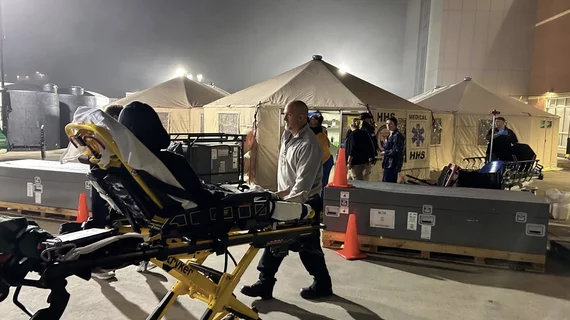


Lessons Learned: Mission Health Hospital Asheville
Impact – 3 days: The initial perception was that the storm’s impact would be minimal. The risks in western North Carolina were not immediately apparent. Three days before the storm, they called in all staff and set up a check-in process. They pre-staged water, food, and generator fuel on site in Asheville. They then began to secure the facility (limiting visitor access) and established a cadence for key hospital officer updates. An Incident Command Center (ICC) was also activated.
Impact + 24 hours: The primary focus was to ensure the safety of patients, staff, and providers. They established which critical infrastructure systems were not functioning, maintained a close watch on food and supplies (aware that water was critically compromised), and worked to reestablish communications channels that had been disrupted (no WIFI and limited cellular). They then conducted an Incident Command Center (ICC) meeting, with limited attendance, to facilitate the start of recovery, and assigned a liaison to manage vertical communication within the facility. Creative problem solving was the focus of the day (water bucket brigade, duct tape, assigned runners for critical duties, supply movement).
Impact days 1 to 2: The team then ensured communication channels were open to stakeholders – city and county government, state and federal agencies, health system network, and non-affiliated hospitals. The ED was prepared for an anticipated surge once the storm passed (unprecedented 275 patients seen in Mission ED). The morgue was prepared for a surge with no way to offload (funeral homes closed); leaders rounded on staff to share information and close gaps in knowledge – combat rumors and disinformation. They approached response in terms of Maslow’s Hierarchy of Need (food, water, rest cycles) — people before hospital operations, and ensured that staff have somewhere to shower, rest (and get hold of their families to let them know what was going on).
Impact days 2 to 4: The goal was to ensure the hospital remains secure as visitors return; to engage infection prevention staff to determine gaps and deficiencies, and determine if the hospitals needed to enact a de-risking plan (evacuating patients to other healthcare sites). The developed specific team and resources for colleague support (employee morale), had to consider a colleague redeployment plan based on hospital needs, and establish a system for staff families to get food, water, and supplies.
Impact days 4 to 7: During this time, it’s essential to recognize that your community relies on your swift response and recovery, and to allow others to assist, as your team is likely exhausted.Teams were divided into A/B groups to allow leaders to rest, shower and simply have a moment. Thing that needed to be considered were transport for anyone who could assist (FEMA, DMORT, DMAT) – how will they get to your site? Leaders had to develop creative housing options – local hotels, AirBnB, and unused hospital campus space; and to think through a sequential way to resume surgical operations – sterie processing and supply systems, emergent/trauma/OB, urgent inpatient and outpatient cases.
Preparing for the next event – Mission Hospital
The teams then had to prepare for the worst but be ready to demobilize quickly (some hospitals in the system were minimally impacted) and have a clearly established “battle rhythm” for ICC and standard scripting available (plug and play). The most vital link to recovery wass dependable, reliable communication (test, test, test), and the knowledge that basic needs must be met before re-establishing any sort of operations. Leaders were given autonomy but had to be rigid in providing status updates. Relationships with vendors were leveraged, including civic organizations and community groups – they want to help (figure out how).
Healthcare Enterprise Response (HCA regional and national efforts)
Before the Storm: Prior to the arrival of the storm, the hospital readiness (27 HCA facilities across 4 divisions in Southern US storm track) was engaged in readiness activities based on individual facility assessments. This included checking the functionality of generators, supplies, and that food stock was adequate. Water tankers and fuel trucks were contracted, incident response teams were activated and de-risking efforts were implemented (patient transfers). HCA Healthcare emergency operations center (EEOC) were activated, with daily briefings being provided to hospitals so they were aware of shortfalls, excess capacity, opportunities, and barriers to moving patients if needed. The focus was on patient safety, and 74 patients in total were transferred from HCA West Tampa and Florida Pasadena hospitals to sister facilities before the storm hit, based on anticipated facility vulnerabilities. Flood mitigation was also initiated – 6500 feet of tiger dam set up at Florida Pasadena hospital (based on prior experience).
North Carolina Response post storm: Road damage cut off Blue Ridge Hospital (Spruce Pine, NC) from ground access and HCA contracted cargo helicopters to make deliveries (2 heavy lift helicopters made 16 runs). Communications were compromised with less than 10% cell service operational at 3 days post-storm, so EEOC set up five Starlink satellite kits to restore hospital connectivity. Five hospitals in North Carolina lost access to community water (including Asheville), and eight weeks post-Helene, they did not have utility-provided potable water; thus, they needed to dig their own wells. To maintain hospital operations HCA deployed tanker trucks to provide water and fuel. Engineers, who were brought from other HCA facilities across the country, troubleshoot on the ground, real-time, innovative solutions to allow water to travel from tankers through to faucets. Portable shower and laundry units were set up for staff and families to use. Generators and tankers were sent to hotels throughout Asheville, allowing staff and their displaced families, as well as responders, to be housed at those sites. Two wells were dug to provide water to cool HVAC units. Two satellite cells on light trucks (COLTs) were brought in to support communication. Sixteen ALS ambulances and crews from outside the area were contracted to help with anticipated transfers, and patients at outlying North Carolina facilities were transferred to Mission Health Asheville for a higher level of care. Some patients who were ready for discharge but had no place to go were transferred to Skilled Nursing facilities and medical centers as they came back online. Hospital staff and volunteers opened “Mini Marts” to provide staff and families with food, cleaning supplies, personal hygiene products, showers, and laundry facilities. Fuel depots allowed staff to fill up cars so as to ensure the ability to get to and from the hospital. Three therapy dogs were brought in as part of the behavioral health teams to help staff, patients, and families deal with the stress of the storm
Preparing for the next big event
The after-action report has over 1000 tasks. Some are simple, others complex and financially unacceptable. Health system and hospitals are working to address the list but have realized that they must prioritize by identifying actions most likely to happen and stratifying interventions by likelihood of impact on the hospital, staff, or community. As 500-year events become increasingly common, now is the time to prepare hospitals, staff, communities, and health systems to respond effectively. Devoting time and financial resources to solutions takes leadership commitment and operational diligence.
